WASHINGTON, USA, (DOD News) – The long-standing wars in Iraq and Afghanistan taught the US military health system to collaborate and innovate research and treatment among the three military services, and, for example, created the combat joint trauma system, a panel of physicians.
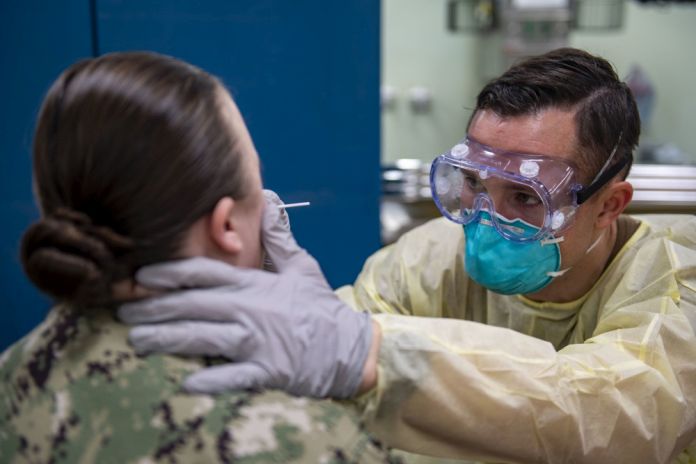
When the COVID-19 pandemic struck the United States this year, that joint trauma system took form almost immediately to gather data on COVID-positive patients in the MHS, Air Force Col. (Dr) Todd Rasmussen, professor of surgery and associate dean of research, Uniformed Services University of the Health Sciences in Bethesda, Maryland, said today during a media roundtable discussion.
Joining Rasmussen on the call were Dr Paul Cordts, chief medical officer for the Defense Health Agency in Falls Church, Virginia; Dr Simon Pincus, director of DHA’s connected health branch; and Army Maj. (Dr) Steven Hong, assistant professor of surgery at the USUHS and chief of head and neck surgical oncology and reconstructive surgery at Walter Reed National Military Medical Center, also in Bethesda.
Rasmussen called the joint trauma center a global system that uses data to monitor care of COVID-19 patients for the center’s established registry to look at and gather data on how best to diagnose and care for patients.
“It’s almost a worldwide [venue] where we go on rounds, but it’s virtual,” he said. “It’s very much like what was done during combat casualty care during the wars, but now it’s more focused on how best to diagnose and manage patients with COVID.”
Using the joint trauma center system in the military and civilian medical sectors, doctors can evaluate their therapies in real-time and adjust clinical practice guidelines, if necessary, toward therapies that appear to be most effective, he noted.
Another innovation MHS pivoted on in the parallels between combat and COVID-19 care is a provider resilience suite of self-care for health care workers. It’s an app that also created useful tips to self-identify signs of burnout and how to deal with it, Pincus pointed out.
Virtual health is another concept that was used in downrange settings, and it is now being used for COVID-19, Rasmussen said. Virtual health is revolutionary for COVID-19, the panel said.
Also, the electronic medical record comes into play with COVID-19. Patients can fill out a questionnaire from home, using the patient portal, and pass it along to their doctor, where a clinical team can review the information and identify patients who are appropriate for COVID-19 testing or those who need further care, Rasmussen said.
“We really want to empower providers and patients digitally to improve the quality of care and health outcomes,” Cordts said. COVID-19 has provided the opportunity in the midst of crisis coverage, and the technologies being used for COVID-19 have potential application for other infectious diseases, too, he added.